AI SOAP Notes for Therapy Practices
The SOAP format, written for talk therapy. Therapy-shaped Subjective and Objective sections, modality-aware Assessment, treatment-plan-linked Plan. Generated during the session, not reverse-engineered from a transcript.

SOAP in therapy is not SOAP in medicine
The same four headings, doing entirely different work.
A medical SOAP note records vitals and exam findings. A therapy SOAP note records affect, mental-status shifts, the modality you used, and the alliance you are tending. Generic medical scribes default to the medical version. Emosapien is built around the therapy version.

| Section | In medicine | In therapy (what Emosapien writes) |
|---|---|---|
| Subjective | Patient-reported symptoms, pain scales, complaints. | Client’s reported affect, presenting concerns, between-session events, what they wanted to bring to the session. |
| Objective | Vitals, exam findings, lab values. | Observed mental-status indicators, affect range, eye contact, engagement, body language, anything you noticed but the client did not name. |
| Assessment | Differential diagnosis, severity, response to treatment. | Modality framing (CBT / ACT / DBT lens), formulation update, therapeutic-alliance shifts, risk assessment, progress against treatment-plan goals. |
| Plan | Medications, follow-up labs, referrals. | Next-session focus, between-session homework, intervention targeted, supervision flag if needed, scheduling. |
Want the full reference for what each section should contain in a therapy progress note? See the complete SOAP notes guide for therapists.
Written during the session, not after
The Assessment is drafted with clinical context already in place.
Most AI SOAP tools generate the note from a recorded transcript. That works for the Subjective and the Objective, but the Assessment ends up generic. A polite paraphrase of what the client said, with the modality framing and intervention timing missing.
Emosapien works the opposite way. The Therapy Agent is in the room while the session happens. It marks when you offered a CBT cognitive-restructuring move, when the client’s affect shifted, when the alliance went rocky and recovered. By the time the session ends, the Assessment already has the clinical context. The transcript is the supporting evidence, not the source.
That is the difference between a SOAP note that reads like a transcript summary and one that reads like clinical work.
Start free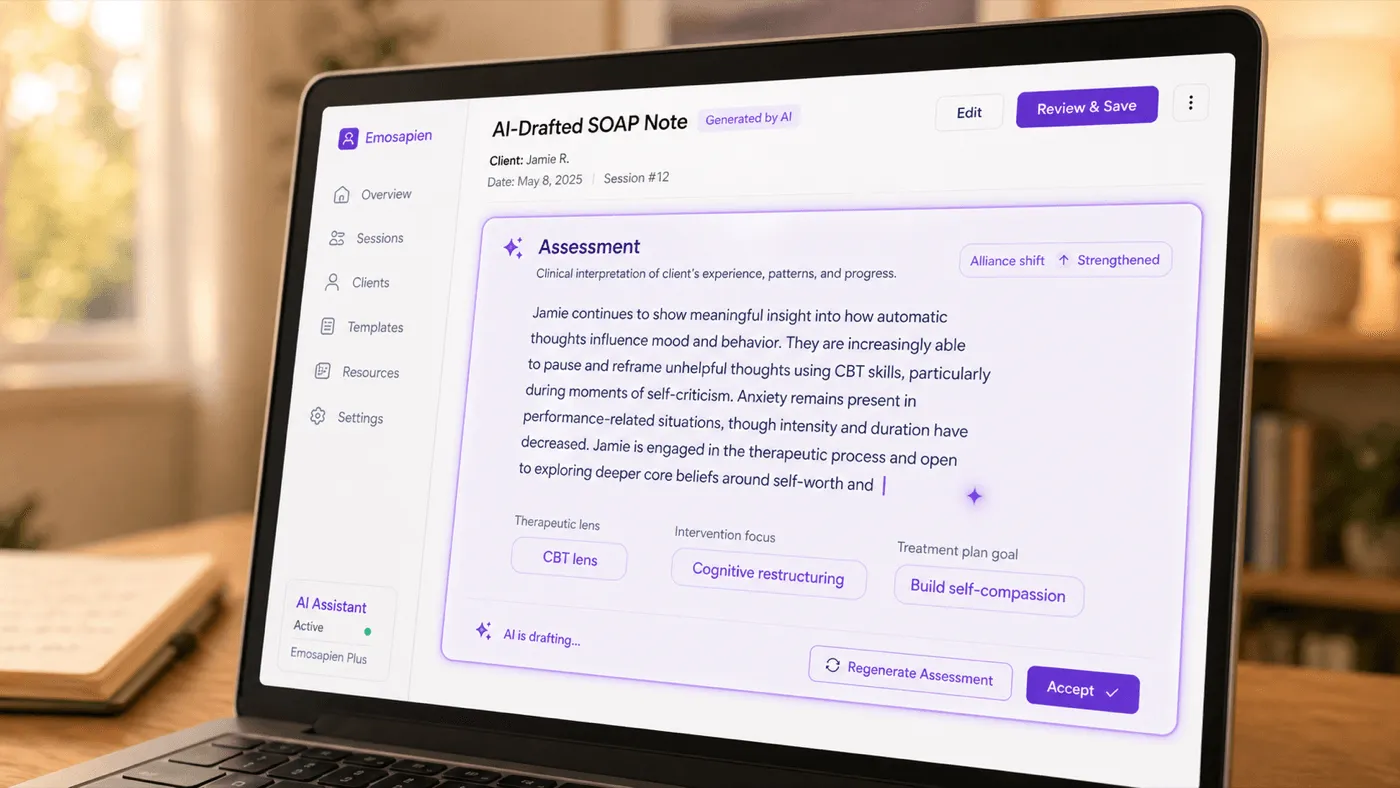
Beyond SOAP
Switch to a different format when SOAP is not the right fit.
SOAP is the default for a reason. But not every caseload uses it. Emosapien switches per client or per session, no template wrangling.
DAP
Data · Assessment · Plan, leaner alternative for case-management workflows.
Format guide →BIRP
Behaviour · Intervention · Response · Plan, standard in addiction counselling and IOP/SUD work.
Format guide →GIRP
Goal · Intervention · Response · Plan, outcomes-anchored progress notes.
Format guide →PIE
Problem · Intervention · Evaluation, still common in clinical-social-work practice.
Format guide →How Emosapien SOAP differs from Upheal, Mentalyc, and Blueprint.
All three are well-built therapy tools. The honest difference is what they put in the Assessment.
| SOAP capability | Emosapien | Upheal | Mentalyc | Blueprint |
|---|---|---|---|---|
| Modality-aware Assessment drafting CBT / ACT / DBT framing carried through the Assessment | Fully supported | Partially supported | Partially supported | Not available |
| In-session intervention prompts feeding the Plan The Therapy Agent surfaces cues live during the session | Fully supported | Not available | Not available | Not available |
| Treatment-plan goals auto-linked to the Plan section Planning Agent maintains continuity across sessions | Fully supported | Partially supported | Partially supported | Fully supported |
| Format breadth (SOAP, DAP, BIRP, GIRP, PIE) PIE adds clinical-social-work coverage on top of the standard four; switchable per client | Fully supported | Partially supported | Partially supported | Partially supported |
| Custom note templates Build and save your own format alongside the standard four | Fully supported | Partially supported | Partially supported | Fully supported |
Why this list excludes general medical scribes. Heidi, Nuance DAX, Suki, Abridge, and Freed all generate excellent medical SOAP notes — but the Assessment they write is a medical assessment, not a therapy formulation. They do not carry CBT, ACT, or DBT framing, do not track the therapeutic alliance, and do not link the Plan back to a treatment-plan goal. Different job.
Trust and compliance
HIPAA-aligned. SOC 2 Type II. ISO 27001.
Session data is encrypted in transit and at rest. Content is never used to train public models. BAA available on Professional and Enterprise. Full posture on the trust page.
See full security posture- ✓ AES-256 encryption at rest, TLS 1.3 in transit
- ✓ SOC 2 Type II audited annually
- ✓ ISO 27001 certified infrastructure
- ✓ No model training on client data
- ✓ BAA included on Professional and Enterprise
- ✓ One-click deletion across backups

The Assessment used to be the section I rewrote completely. Now I tweak two sentences. The modality framing is already there, the alliance shift is captured, the plan links to the goal. I save the half hour.
Frequently asked questions
The structure is the same; the content is not. Medical SOAP captures vitals, exam findings, and lab values. Therapy SOAP captures affect, mental-status indicators, modality framing (CBT/ACT/DBT), formulation updates, and therapeutic-alliance shifts. Emosapien is built for the second one. The full breakdown lives in the SOAP notes guide.
All four sections, with the Assessment carrying the heaviest clinical weight. The Therapy Agent tracks which intervention you used and the client’s response in real time, and the Scribe Agent writes that into the Assessment with modality-specific framing. You read it, edit it, and sign it. Most therapists make small wording edits, not rewrites.
SOAP is the default, but DAP, BIRP, GIRP, and PIE are all supported and switchable per client. BIRP is the right choice for SUD and IOP work; GIRP fits outcome-anchored practices. The documentation hub has format-by-format guides.
Accurate enough that most clinicians edit lightly rather than rewrite. The accuracy comes from the in-session context the Therapy Agent collects: modality cues, intervention timing, client response. Not from a transcript alone. You always sign the final version, so clinical judgment stays with you.
Yes. SOC 2 Type II audited, ISO 27001 certified, BAA available on Professional and Enterprise. Session content is never used to train public models. See Trust and Security for the full posture.
Yes. Direct integrations with SimplePractice, TherapyNotes, Jane, and Halaxy ship structured SOAP. HL7 / FHIR export is also available. Custom EHR connectors are part of the Enterprise plan.
Yes. The free plan covers 10 sessions per month with full SOAP generation, no credit card required. Start free.
Therapy SOAP notes that read like clinical work.
Free for 10 sessions per month. No credit card. Start tonight, write your next session’s note tomorrow.
Start free